

Introduction
Lupus is a complex autoimmune disorder that can significantly impact a person’s life expectancy. For many, the unpredictability of the disease and its flare-ups often lead to concerns about how long they will live with lupus. While lupus was once considered a fatal diagnosis, advances in treatment and early detection have drastically improved survival rates. However, lupus still presents challenges, especially with complications like heart disease, kidney failure, and infections, which can reduce life expectancy. In this article, we’ll explore five essential facts about lupus life expectancy to help you understand the factors that influence how long someone with lupus can live, and the practical steps to extend life expectancy.
1. Understanding lupus and life expectancy


It is an autoimmune disorder in which the immune system mistakenly attacks joints, skin, kidneys, and other tissues. Because its symptoms come and go unpredictably, many people worry about their life expectancy with lupus. With early diagnosis and treatment, most patients enjoy a typical or near‑normal lifespan. However, serious lupus complications, including heart disease, kidney failure, and infections, still claim lives. About 10–15 % of people die prematurely, so understanding risk and acting proactively can make a real difference.
2. Historical perspective on lupus longevity


Lupus was often fatal decades ago. In the 1950s, only half of patients were alive 5 years after diagnosis. Corticosteroids, immunosuppressants, and biologics changed all that: more than 90% of people live 5 years, and 85-90% live 10 years. Today, about 75% are still alive 20 years after diagnosis. These milestones are proof of the advances made in medicine and the decrease in the death rate from lupus, although long-term complications continue to accumulate.
3. Factors influencing lupus life expectancy


Sex and gender
About 90 % of people with lupus are women, but men who develop SLE often have more severe disease. Regardless of sex, early recognition and treatment improve the average lifespan of people with lupus.
Age at diagnosis
The age at which a person is diagnosed with lupus has a big impact on their life expectancy. Juvenile‐onset SLE is aggressive, with children and teens having more flares and organ damage and often on long-term steroids. Late-onset lupus is less severe but complicated by hypertension, diabetes, and other chronic illnesses. Those diagnosed after age 50 are about five times more likely to die within a decade.
Race and ethnicity
Race and ethnicity shape the life expectancy for lupus disease. Lupus is two to three times more common in African American, Hispanic, Asian, Native American, and Pacific Islander communities, and these groups develop more active disease. Black people with lupus have higher death rates and die more than 10 years earlier on average due to socioeconomic factors.
Organ involvement and complications
Certain organs, when affected, markedly reduce life expectancy for lupus disease:
- Kidneys and heart: Up to 60 % of patients develop lupus nephritis, and people with lupus are two to ten times more likely to develop heart disease. These organ complications raise mortality, but those with nephritis still achieve high five‑ and 20‑year survival rates.
- Infections. Immunosuppressive drugs control the flares, but they do weaken the immune system. Severe infections account for about a third of lupus deaths, and steroids increase the risk of respiratory, skin, and urinary infections.
- Cancer and other conditions. Cancer, end-stage renal disease, and infection continue to be important causes of death. Women with lupus are more prone to pregnancy complications like miscarriage and preeclampsia, but with proper planning, the risk factors can be lowered.
Summary of key risk factors
The table below shows how demographic and clinical factors impact life expectancy in lupus. We are all different, but knowing these patterns can help tailor care.
Factor Impact and notes:
- Sex: Women make up about 90 % of patients; men tend to have more severe disease and lower survival.
- Age at diagnosis. Juvenile‑onset lupus is aggressive; late‑onset is milder but complicated by comorbidities, and late‑onset reduces survival.
4. Common causes of death in lupus patients
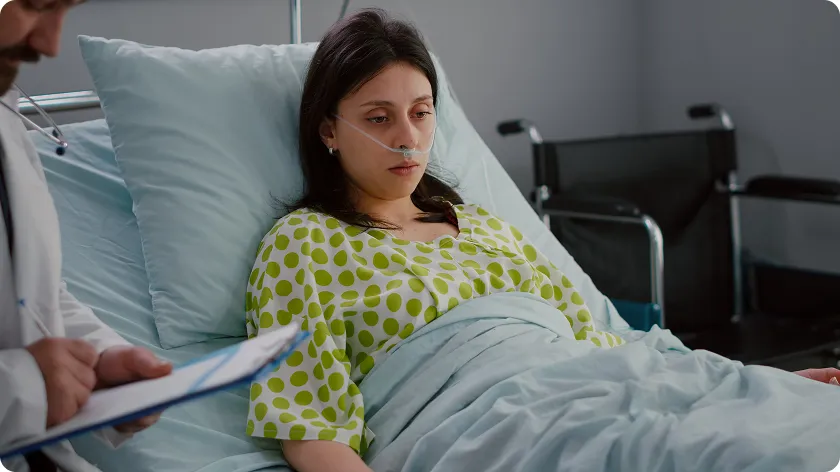
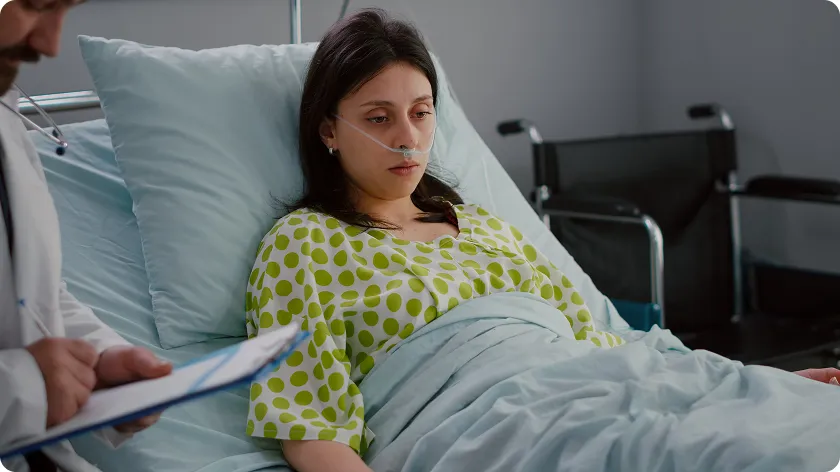
Even with modern treatments, several complications are still responsible for the lupus death rate and shorten the lifespan of lupus patients:
- Heart, kidney, and infections: Lupus-related inflammation and steroids accelerate atherosclerosis and scar the kidneys, and immunosuppression means infections cause about one-third of lupus deaths.
- Cancer, other illnesses, and disparities: Cancer and other chronic diseases contribute to mortality, and socioeconomic factors such as poverty and discrimination increase death rates.
5. Practical steps to improve life expectancy


Managing lupus successfully involves both medical treatment and healthy lifestyle habits. The following strategies may help reduce complications and support long-term health.
Work Closely With Your Healthcare Team
Take medications exactly as prescribed and attend regular check-ups. Consistent monitoring can help prevent flares and reduce the risk of long-term organ damage.
Stay Heart-Healthy
Regular exercise, a balanced diet, and avoiding smoking can lower the risk of cardiovascular disease, which is more common in people with lupus.
Avoid Flare Triggers and Infections
Protect yourself from excessive sun exposure, stay up to date with vaccinations, and reduce exposure to infections whenever possible.
Support Mental and Reproductive Health
Managing stress through counselling, therapy, or support groups can improve emotional well-being. Pregnancy planning with your healthcare team is also important for safer outcomes.
Stay Active and Monitor Symptoms
Physical activity and early recognition of new symptoms can help minimise complications and improve overall quality of life.
Living with lupus can be challenging, but combining medical care with healthy daily habits may improve both quality of life and long-term outcomes.
FAQ
1. How long do people with lupus live?
Most patients now live near‑normal lives. Survival exceeds 90% at 5 years and 85% at 10 years.
2. Is lupus life‑threatening?
Lupus can be life‑threatening when organ damage or infection occurs, and about 10–15 % of patients die prematurely, but with treatment and healthy habits, most live long lives.
3. How does lupus kill you?
Lupus itself is not fatal; complications are. Heart disease, kidney failure, infections, and cancer cause most deaths.
4. Can you die from lupus?
Yes, despite improved survival, 10–15 % of patients die prematurely, especially those with severe disease or limited access to care.
5. What kills lupus patients?
Heart disease, kidney failure, infections, and sometimes cancer are the main culprits. Social factors such as poverty and racial disparities also play a role.
Conclusion
Lupus is complex but no longer a death sentence. Thanks to modern therapies, most patients, especially those diagnosed early and treated promptly, can live decades beyond their diagnosis. Still, the average lifespan and life expectancy for lupus disease depend on vigilance: demographic factors and complications such as heart disease, nephritis, and infections continue to drive mortality.
That is why I have always been proactive in my lupus longevity. Work with your health care team. Take your medications as directed. Live a heart-healthy lifestyle. Protect yourself from infections and the sun. Mental health, social support, and advocacy may affect outcomes. It is also important to manage stress and get equitable care.
Internal Links
- Arthritis in Fingers: 7 Essential Signs & Relief Tips
- Arthritis in hands: 7 Effective Signs & Relief Tips
- 8 Essential Lupus Nephritis Symptoms to Know
External Links
- Essential Lifespan Lupus: Life Expectancy Explained
- Prognosis and Life Expectancy
- Life expectancy and prognosis with lupus
References
- March 2023 | Pain And Spine Care https://www.painspinecenters.com/2023/03/




