
Introduction
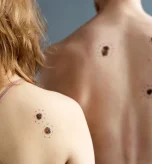
Skin cancer is alarmingly common. More people are diagnosed with it every year than with any other cancer. In fact, at least 1 in 5 people will develop skin cancer by age 70, and about 9,500 Americans are diagnosed each day. Understanding the 3 types of skin cancer is crucial because early detection can save lives. Even though the most common skin cancers (basal cell carcinoma, squamous cell carcinoma, and melanoma) often start as harmless spots, ignoring warning signs can be dangerous.
By the end of this article, you’ll know how to recognize each skin cancer type, understand how a skin cancer diagnosis works, and learn prevention steps like sun protection and regular self-checks. This knowledge will help you protect your skin and act fast on any concerning changes.
The 3 Main Skin Cancer Types
Basal and squamous cell carcinomas originate in different layers of the skin and account for the majority of cases. At the same time, melanoma arises in pigment cells and is rarer but much more dangerous if it spreads. Understanding how each type looks and behaves is key. Below, we look at each type’s appearance, risks, and outcomes.

1. Basal Cell Carcinoma (BCC)
Basal cell carcinoma is the most common skin cancer, caused primarily by long-term UV exposure. It starts in the basal cells (deep layer of the epidermis). BCC often looks like a shiny, pearly bump or flat scaly patch, sometimes with tiny blood vessels on its surface. It may be pink, skin-colored, or translucent and usually appears on sun-exposed areas (the face, ears, and neck).
BCC grows very slowly and rarely spreads. Simple removal cures it in nearly 100% of cases. If left untreated, BCC can still cause local damage (a sore that keeps growing or bleeding).
- Appearance: Pearly/shiny bump or flat scaly patch on sun-exposed skin.
- Action: See a doctor about any new or non-healing spot. Early removal is usually curative.
2. Squamous Cell Carcinoma (SCC)
Squamous cell carcinoma arises from squamous cells (the outermost layer of the epidermis). SCC often appears as a firm, red bump or a rough, scaly patch that may crust or ulcerate. It usually appears on sun-exposed skin (hands, arms, face). Compared to BCC, SCC grows faster and can spread if untreated.
SCC is mainly caused by UV damage. Early SCC is usually cured by removal, but untreated SCC can be life-threatening.
- Appearance: Red scaly patch or firm nodule (may ulcerate) on sun-damaged skin.
- Risk & Spread: Caused by UV damage; it can invade nearby tissue and lymph nodes.
- Action: Have any persistent, thick, or non-healing spots checked. Early removal prevents spread.
3. Melanoma
Melanoma is the deadliest skin cancer, starting in pigment cells. A melanoma often looks like a new or changing mole with irregular color and uneven borders. Look for the ABCDE warning signs (Asymmetry, Border irregularity, Color variations, large Diameter, Evolving size). Melanomas can be brown, black, or even pink/white and may appear on normal-looking skin.
Melanoma grows deep and spreads quickly. It’s mainly driven by intense UV exposure (especially sunburns). Early removal is critical: an early melanoma has about a 99% cure rate, but once it spreads to lymph nodes or organs, 5-year survival falls to around 35%.
- Appearance: Irregular, multicolored mole or spot (ABCDE rule). Look for uneven edges or multiple colors.
- Risk: Mainly UV-induced; fair skin or many moles raise your risk.
- Action: See a doctor for any new or changing mole. When in doubt, get a biopsy.
Table: Main features of the 3 skin cancer types.
| BCC | Pearly bump or scaly patch | Very low | Most common (~80%) | ~100% (when removed) |
| SCC | Red scaly patch or nodule | Low/moderate | 2nd most common | ~95% (when removed) |
| Melanoma | Irregular pigmented mole | High | ~10% of cases | ~99% (early); ~35% (metastatic) |
Prevention and Early Detection
The good news is that many skin cancers are preventable and highly curable when caught early. Simple daily habits can slash your risk. For example, using SPF 30+ sunscreen every day cuts melanoma risk by about half. Below are key steps for self-exams, sun safety, and medical checks to help prevent skin cancer and catch it early.


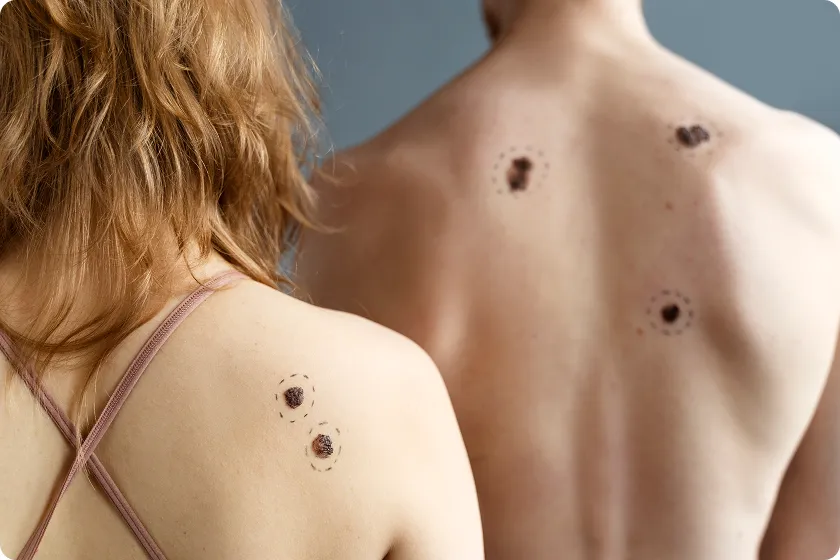
Self-Exams: Know Your Skin
Check your skin every month in a well-lit room. Examine your entire body (front, back, arms, legs, face, ears, scalp, between toes) using mirrors or a partner.
- Inspect: Use the ABCDE rule on each mole during your exam (Asymmetry, Border, Color, Diameter, Evolving).
- Track: Photograph or note any new or changing spots over time.
- Action: If you find a new, growing, or changing lesion, see a doctor promptly. Even a tiny early melanoma is usually curable.
Sun Safety: Protect Your Skin
UV radiation is the main cause of skin cancer, so protective habits drastically reduce risk. Use a broad-spectrum sunscreen (SPF 30 or higher) on all exposed skin daily, even on cloudy days. Reapply every 2 hours and after swimming/sweating. Wear sun-protective clothing (long sleeves, wide-brim hats, UV-blocking sunglasses) outdoors. Seek shade when possible and avoid tanning beds completely. One indoor session can equal many sunburns.
- Cover up: Wear long sleeves, wide-brim hats, and UV-blocking sunglasses when outside.
- Sunscreen: Apply SPF 30+ daily and reapply often (every 2 hours or after swimming or sweating).
These habits are proven: daily SPF use can cut melanoma risk by ~50%, and simply covering up can literally save your life.
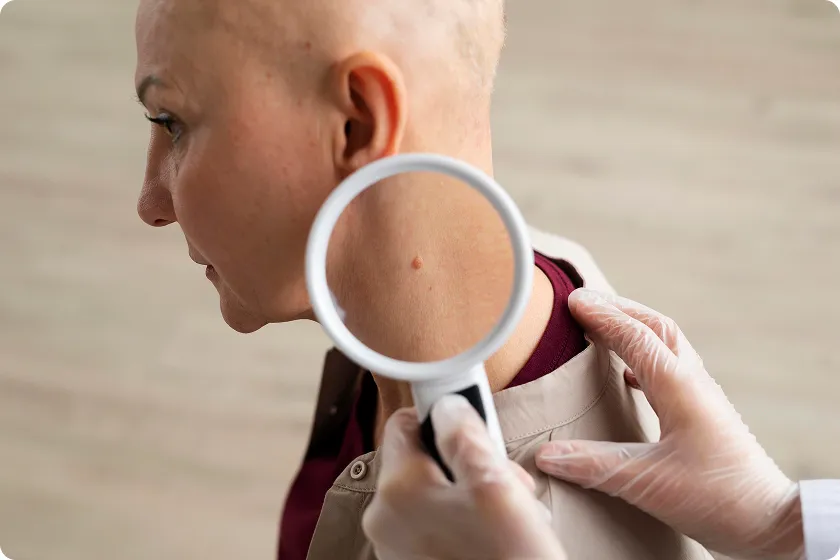
Professional Exams and Diagnosis
If you or your doctor find a suspicious spot, a dermatologist will examine it (often with a dermoscope) and then perform a biopsy (removing part or all of the lesion for testing). If melanoma is diagnosed, further scans or a sentinel lymph node biopsy are performed to determine if it has spread. Here are the key steps in a typical skin cancer diagnosis:
Table: Steps in skin cancer diagnosis.
| Skin exam | Tissue sample (shave, punch, or excision) |
| Dermoscopy | Magnified, lighted exam of the lesion |
| Biopsy | Tissue sample (shave, punch or excision) |
| Imaging | Scans (ultrasound, CT, etc.) to check spread, if needed |
Each step leads to an official diagnosis and staging, which guides treatment. Remember: when in doubt, get a spot checked. Even benign-looking moles can hide cancer, and a biopsy is the surest way to diagnose skin cancer.
FAQ
1. What are the three types of skin cancer?
They are basal cell carcinoma, squamous cell carcinoma, and melanoma, the three major skin cancers arising from different cells. Basal and squamous cell cancers (non-melanoma) are the most common, while melanoma is less common but far more dangerous. These types differ in appearance and risk.
2. What are the four types of skin cancer?
The four common types are basal cell carcinoma, squamous cell carcinoma, melanoma, and Merkel cell carcinoma. Merkel cell is a rare, aggressive skin cancer (~3,200 US cases/year) that is more dangerous than the others.
3. How is skin cancer diagnosed?
Doctors diagnose skin cancer by examining your skin and confirming with a biopsy. A dermatologist inspects suspicious moles (often using a dermatoscope) and removes a sample for lab testing. If melanoma is found, additional imaging or lymph node tests may be done to check for spread.
4. How does skin cancer kill you?
Skin cancer is deadly when it spreads to vital organs. For example, melanoma that spreads to the brain, lungs, or liver causes organ failure or fatal complications. An untreated squamous cell carcinoma that spreads to lymph nodes can also be lethal. This is why early detection of skin cancer is lifesaving.
Conclusion
In summary, the 3 types of skin cancer (basal cell, squamous cell, and melanoma) differ in appearance and severity. Basal cell is the most common and least dangerous, SCC is moderate risk, and melanoma is rare but the most deadly if it spreads. Key takeaways: check your skin regularly, use sun protection, and have any suspicious spots examined. Early skin cancer diagnosis (via exam and biopsy) gives nearly 100% cure rates for local disease, while delays can let it become life-threatening. Understanding skin cancer stages and acting on changes empowers you to avoid serious outcomes.
Stay protected: Wear sunscreen daily, cover up, and avoid tanning. Make skin checks part of your routine and encourage others to do the same. Share this post to help spread awareness. Have questions or personal stories? Comment below. For more in-depth guidance, see our comprehensive pillar post on skin health and prevention.
Internal Links
- Understanding Blood Pressure Readings: 6 Essential Facts You Must Know
- Sinus Infection: 7 Proven Ways to Relieve Jaw Pain and Dizziness
- Can Constipation Cause Fever? 7 Essential Causes of Fever with Constipation
External Links
Reference
- 5 WAYS TO PROTECT YOUR SKIN FROM THE SUN – Totality Medispa and Skincare https://totality-skincare.com/en-gb/blogs/tips-tricks/5-ways-to-protect-your-skin-from-the-sun
- Reconstructive Procedures | Hancey Plastic Surgery | Sandy UT https://www.jasonhanceymd.com/reconstructive/
- Ishihara, T., Nakamura, A., Kageshita, T., & Ono, T. (2001). Sentinel Lymph Nodes Study in 30 Cases of Melanoma. The Journal of Dermatology. https://doi.org/10.1111/j.1346-8138.2001.tb00148.x
- Medicine and Technology: July is UV Safety Month https://www.medicineandtechnology.com/2011/07/july-is-uv-safety-month.html
- Bioderma Photoderm Nude Touch Mineral Tintée SPF 50+ | Loolia Closet https://looliaclosets.com/products/photoderm-nude-touch-mineral-tintee-spf-50
- The Importance of Early Skin Care in Cancer Prevention – Arlington Dermatology https://www.arlingtondermatology.net/2014/03/20/the-importance-of-early-skin-care-in-cancer-prevention/
- Ishihara, T., Nakamura, A., Kageshita, T., & Ono, T. (2001). Sentinel Lymph Nodes Study in 30 Cases of Melanoma. The Journal of Dermatology. https://doi.org/10.1111/j.1346-8138.2001.tb00148.x
- (2019). Abstracts and Case Studies From the College of American Pathologists 2019 Annual Meeting (CAP19). Archives of Pathology & Laboratory Medicine, 143(9), E2-E226.
- Ishihara, T., Nakamura, A., Kageshita, T., & Ono, T. (2001). Sentinel Lymph Nodes Study in 30 Cases of Melanoma. The Journal of Dermatology. https://doi.org/10.1111/j.1346-8138.2001.tb00148.x
- Skin cancers – Cosmetic Enclave https://drtayyabplasticsurgeon.com/services/skin-cancers/
- Ishihara, T., Nakamura, A., Kageshita, T., & Ono, T. (2001). Sentinel Lymph Nodes Study in 30 Cases of Melanoma. The Journal of Dermatology. https://doi.org/10.1111/j.1346-8138.2001.tb00148.x
- Ishihara, T., Nakamura, A., Kageshita, T., & Ono, T. (2001). Sentinel Lymph Nodes Study in 30 Cases of Melanoma. The Journal of Dermatology. https://doi.org/10.1111/j.1346-8138.2001.tb00148.x1